A Story of Health Equity
By Drew Thomas:
I’d like to highlight a facet of my – geared around journey through “Health Equity”. This is a concept we are often referencing but drawing the correlation of how this manifests itself is not always as easily identifiable. So, I am going to share my personal “mission/survivor story”, and how it relates to health equity. It’s going to be focused around – “My Parents” – Particularly my father. The short version of the story which I most often share is – I lost both of my parents due to illnesses, most recently, my father died of a heart attack 4 years ago. But really that only tells a fraction of the story.
My parents, Phil & Karen Thomas. We lived 80 miles SW of Chicago in what is referred to as the “Illinois Valley”. All things considered were a relatively normal family. I was their only child. In 2005 – when I was 15, my mother developed Breast Cancer, and ultimately passed away in 2008. This is m y mother, on what was her last photographed image. This is when she was on Hospice – She graduated with her master’s degree about 1 week before she passed. She was informed she had developed stage 4 breast cancer. Stage 4 Cancer may seem like a common occurrence – but where the inequities lie, because of where we lived, without access to proper healthcare – cancer centers that were not taking new patients in my small town. It wasn’t until her first trip to see a specialist where she was given 3 months to live. Death from cancer was the outcome – but in reality, this was an equity issue.
y mother, on what was her last photographed image. This is when she was on Hospice – She graduated with her master’s degree about 1 week before she passed. She was informed she had developed stage 4 breast cancer. Stage 4 Cancer may seem like a common occurrence – but where the inequities lie, because of where we lived, without access to proper healthcare – cancer centers that were not taking new patients in my small town. It wasn’t until her first trip to see a specialist where she was given 3 months to live. Death from cancer was the outcome – but in reality, this was an equity issue.
My father was there every step of the way. He was really a rock star throughout the process. My father who for a long time dealt with Diabetes, hypertension fell very ill within 1 year of Karen’s passing.
This was him – my freshman year of college, the year I first moved to Texas – to go to school/play football at UTEP. And this is where the story really begins. At the beginning of his health journey. I remember being at the doctor’s office (in Illinois) when he was getting read his diagnoses and developed a game plan with his primary healthcare doctor. His doctor said, “you are going to need to see a blood & bone specialist.” There were very few specialists like this in the area we lived in.
And this is where the story really begins. At the beginning of his health journey. I remember being at the doctor’s office (in Illinois) when he was getting read his diagnoses and developed a game plan with his primary healthcare doctor. His doctor said, “you are going to need to see a blood & bone specialist.” There were very few specialists like this in the area we lived in.
The Primary Care Doctor shared with us, when making the referral – “Now I am going to be very honest with you and share that they have been known to not take in – people of color”. He said, “I’d still refer you, but just wanted to let you know that”. That day – we were not admitted to see any specialists that were in our area (when they found out his skin color). I know I’m providing a lot of contexts, but this key detail proved to be very troublesome for my father’s health journey moving forward. The closest specialist was 45 miles away, and very difficult to get to.

His condition worsened; he lost his ability to drive & to walk. He could get around a little bit on a walker but was a major fall risk. He was so big – if he fell nobody could pick him up. At that point, we needed to admit him into an assisted living facility. In Chicago, 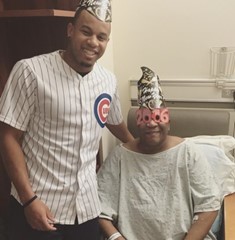 without easy access to healthcare and the stress that racism caused, small issues were compounded into large ones. And large issues were presenting fatal outcomes. These are structural barriers.
without easy access to healthcare and the stress that racism caused, small issues were compounded into large ones. And large issues were presenting fatal outcomes. These are structural barriers.
And to just keep it all the way real – We didn’t have any money. This process had bled us dry financially. As the conditions progressed, and got more complex, his insurance rates rose to a point where we could no longer afford the assisted living facility where he was eventually evicted.
(Image to the right, 2017) – This is him on his last day, when I went to help him move out of his facility. Where ultimately again – I had to watch my father be refused care and asked to fend for himself. He couldn’t walk, he had developed a form of Alzheimer’s, he was on Kidney Dialysis, and his diabetes & hypertension were as rough as ever.
fend for himself. He couldn’t walk, he had developed a form of Alzheimer’s, he was on Kidney Dialysis, and his diabetes & hypertension were as rough as ever.
You know – when I look at this picture, it almost looks like an end but all I see is the journey. Within 3 weeks of his eviction, and off that level of care, he passed away from a heart attack.
Like I said earlier – we were a pretty normal family, and my father was a pretty incredible man who deserved a better health outcome. Why did his quality of life have to be so difficult? How are many people’s health journeys influenced by where they live? How many are influenced by the color of their skin?
 Ultimately – all of this ties back to the concept of “Health Equity”. When we talk about an equitable approach.
Ultimately – all of this ties back to the concept of “Health Equity”. When we talk about an equitable approach.
The AHA funds programs – specifically to support Women’s health.
The AHA funds & supports research geared around battling Chronic Conditions.
The AHA funds & supports Advocacy Teams across the country – that have the ability to go out and threaten the constructs of structural racism.
Why I walk, why I work at the AHA, why I stay active in the Black Community –is because there is still a tremendous amount of work to be done in bridging the equitable gaps.
– Drew Thomas
 Drew’s Thomas, Vice President, Development at AHA
Drew’s Thomas, Vice President, Development at AHA
Drew currently serves as the Vice President of Development at the AHA in Austin, TX, and the Vice President of Health & Wellness of the 100 Black Men of Austin.
(The 100 Black Men of Austin is a volunteer/mentorship organization comprised of prominent men of color in the Austin, TX. The group is committed to the intellectual development of youth, educational opportunities for all, and the economic empowerment of the African American Community).
Prior to joining the AHA, Drew worked in leadership for a non-profit organization that provided resources for Children in foster care across the U.S.
Drew earned his B.A and M.S from the University of Texas at El Paso (UTEP) where he was also a 4-year letter winner and Team Captain of the football team.